
One of the first lung transplant patients to have a skin patch from their donor grafted onto them in a bid to spot organ rejection faster has hailed the method for helping him get swifter treatment.
Darren White was given steroids when tests showed his body was rejecting his new lung three months after his transplant.
More than a year on, the 53-year-old is doing well and said he can be “more of a dad” to his toddler because he is able to walk and take him to the park.

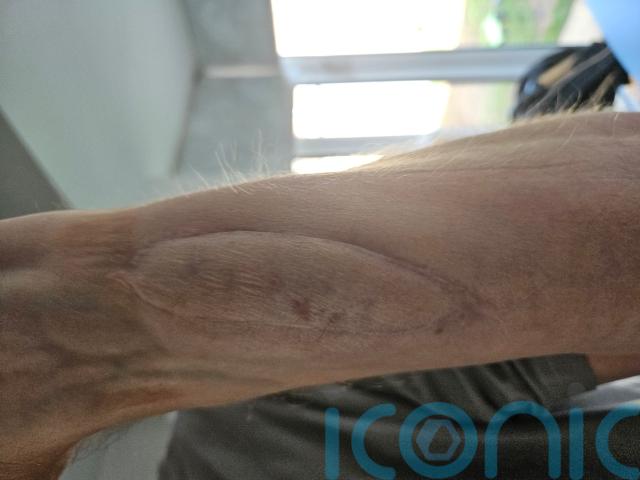
Experts leading the Sentinel trial said the skin patch, which is grafted onto the forearm of patients at the same time as their lung transplant, acts as a “window”.
Scientists believe the skin rejects earlier than other organs and is more visible, meaning medics can treat rejection as soon as a rash appears and slash the risk of permanent damage.
So far, 10 patients have received 10cm by 3cm skin patches from their organ donor as part of the study.
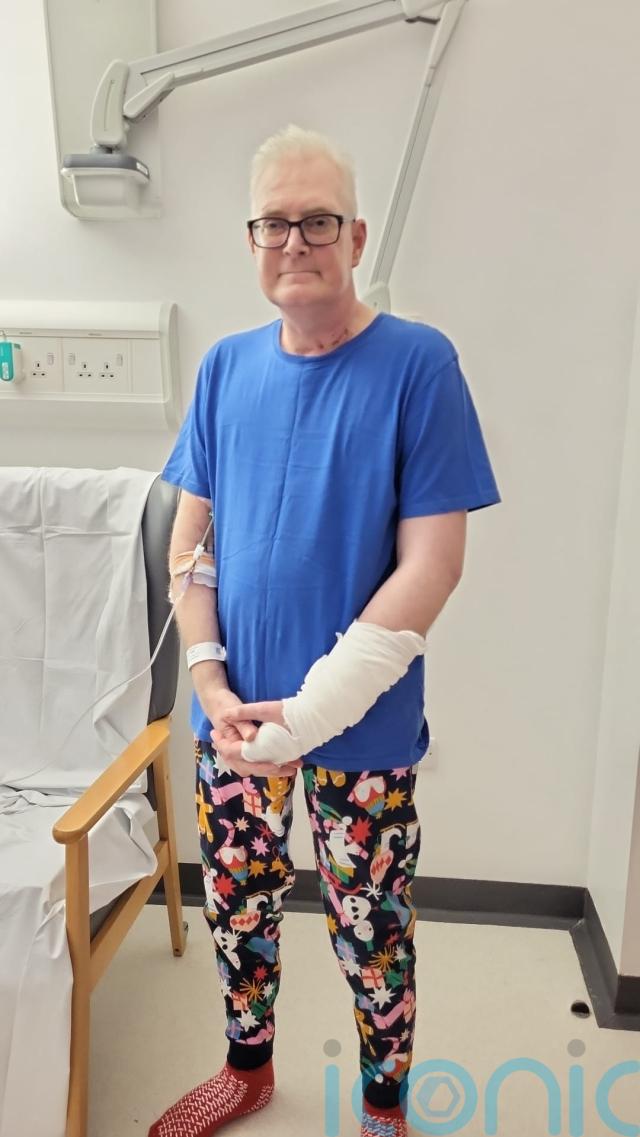
Mr White, a former bus driver from Stockton-on-Tees, had a lung transplant in late 2024.
Earlier the same year he was diagnosed with lung fibrosis, which causes the lungs to become scarred and makes breathing difficult.
He said he did not hesitate to say yes when approached about the Sentinel trial while on the waiting list.
“Anything that might help to avoid rejection was worth a try,” Mr White said.
“Rejection is the biggest fear of any transplant recipient, so having something that might be able to catch it much sooner than otherwise, was really appealing.”
According to NHS Blood and Transplant (NHSBT), lung rejection is hard to detect as it can involve blood tests, biopsies and X rays.
Rates of rejection are highest in the first three to six months post-surgery, and happen in almost a third of patients.
Three months after having his transplant, Mr White noticed a purple rash on the skin patch and sent photos to medics.
A biopsy showed mild rejection and he was treated with steroids.
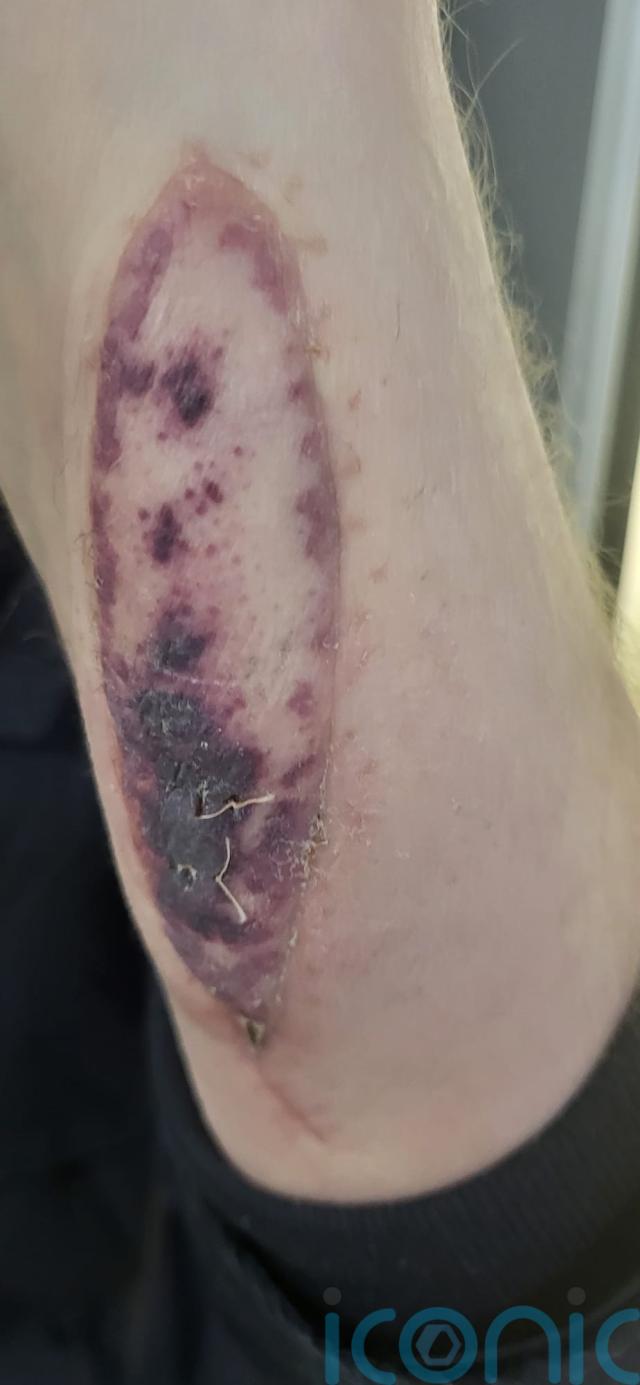
“I definitely believe the skin patch helped to stop the lungs from being rejected,” Mr White said.
“I was feeling fine, there was no reason for me to think that the lungs were being rejected, the only sign was the rash.
“I’m over a year post-transplant now and doing really well. Who knows if that would be the case if the rash hadn’t shown up and rejection wasn’t spotted until further down the line.”
Mr White, who is a father to Daniel, three, said he hopes the trial shows skin patches are a viable way of detecting organ rejection early.
Speaking about life post-transplant, he said: “The biggest difference is I can walk, I can take Daniel to the park to play. Before he could sit on my knee, drive my buggy but that was it, I couldn’t do much with him. I can be more of a dad now.
“My favourite thing is to go to the park, Daniel always asks to go on the swing and we have one in our garden. I can push him now. It’s the simple things that are the best, we both love it.”
The Sentinel trial is set to run until 2027 and will recruit 152 patients at five centres; Freeman Hospital, Harefield Hospital, Queen Elizabeth Hospital, Royal Papworth and Wythenshawe Hospital.
The skin grafts are carried out by plastic surgeons at the University of Oxford.
The method has been used previously in patients receiving intestinal transplants.
The families of donors must consent for the skin transplant to take place via NHSBT specialist nurses.
Henk Giele, chief investigator of Sentinel and an Oxford plastic surgeon said: “It seems logical that having a window to your transplant can provide an early warning system of rejection or reassure you that you don’t have rejection but we have to prove it works.
“We are so grateful to the patients, the donors and their families, the transplant teams, and the NHSBT staff who make this important trial happen. We hope it will change what we know about transplant and makes patients lives better and longer.”
Andrew Fisher, a professor of respiratory transplant medicine at Newcastle University, honorary consultant respiratory physician at Newcastle Hospitals and the lead for Sentinel in Newcastle, added: “If successful, this approach has the potential to revolutionise the way lung transplants are performed in the future and reduce the problems with detecting and treating rejection early, which is vital.”
Emma Lawson, organ donation innovation and research lead at NHSBT, added: “Thanks to the generosity of amazing donor families providing additional consent for skin grafts, patients are now receiving them and we are privileged to work alongside them to enable this important trial to go ahead.”
Subscribe or register today to discover more from DonegalLive.ie
Buy the e-paper of the Donegal Democrat, Donegal People's Press, Donegal Post and Inish Times here for instant access to Donegal's premier news titles.
Keep up with the latest news from Donegal with our daily newsletter featuring the most important stories of the day delivered to your inbox every evening at 5pm.